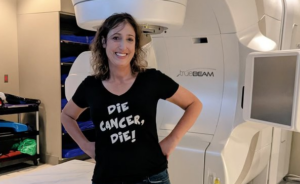
The stories below come from people whose lives have been touched by lung cancer. In addition to providing unique insight on what it’s like to battle and live with the disease, each story also provides reasons to be hopeful about the future of lung cancer research.
- GlennaBiomarker testing opens possibilities for treatment
- LexiChanging the conversation about lung cancer
- LaurenFitness training injury leads to young mom’s diagnosis
- BillAfter biomarker testing, ‘there was actual hope’
- SuzanneFinding hope by connecting with other ALK+ patients
- Donna‘I realized I did have a future’
- JoanneMoving beyond blame, focusing on peace and gratitude
- CarolineLung cancer across three generations of women
- JeffGetting busy living, despite stage 4 diagnosis
- MarleyFatigue wasn’t just acid reflux or part of being a young mom
- XavierVeteran raises awareness of lung cancer in the military
- JulieA mammogram leads to an early-stage lung cancer diagnosis
- TejalFacing lung cancer with a new mantra: breathe easy and fight hard
- AmyArmed for the fight with information and support
- Christine‘Cancer is hard’ – and having support makes all the difference
- WendyManaging lung cancer as a chronic illness
- GerriHaving adventures and living her best life with stage 4 EGFR+ NSCLC
- MaureenStage 4 KRAS+ patient “doesn’t have time for lung cancer”
- JennRunning for research after a lobectomy
- KarenFeeling as confident about her Stage 4 diagnosis as she did with Stage 2
- ColleenPromoting education on risks and symptoms “because lives truly depend on it”
We remember…
LCRF honors and remembers those who have graciously shared their stories with us and have since passed away. By telling about their experiences, they helped – and continue to help – those who are navigating their own diagnoses.